Posts for: July, 2019
While braces are often the stars for straightening smiles, they're not the only cast members in an orthodontic production. Orthodontists occasionally turn to other appliances if the bite problem is challenging. Whatever the tool, though, they usually have something in common—they use the principle of anchorage.
To understand anchorage, let's first consider the classic kid's game Tug of War. With teams on either end of a rope, the object is to pull the opposing team across the center line before they pull you. To maximize your pulling force, the player at the back of your rope, usually your stoutest member, holds steady or "anchors" the rest of the team.
Like a Tug of War team, braces exert force against the teeth. This stimulates the supporting periodontal ligament to remodel itself and allow the teeth to move. The braces use the teeth they are attached to as anchors, which in a lot of cases are the back teeth. By attaching a thin wire to the brackets or braces on the teeth, the orthodontist includes all the teeth on the arch, from one end to the other. Anchored in place, the wire can maintain a constant pressure against the teeth to move them.
But not all bite situations are this straightforward. Sometimes an orthodontist needs to influence jaw growth in addition to teeth movement. For this purpose, they often use orthodontic headgear, which runs around the back of the head or neck and attaches to orthodontic brackets on the teeth. It still involves an anchor but in this case it's the patient's own skull.
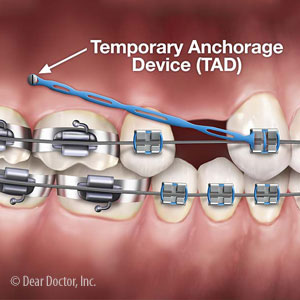
In some situations, an orthodontist may feel he or she needs more anchorage as the teeth alone may not be enough. For this, they might establish a separate or additional anchor point using a temporary anchorage device (TAD). A TAD resembles a tiny screw that's inserted into the jawbone near the tooth intended for movement. The orthodontist can then attach the TAD to braces hardware using some form of elastics. After treatment, they remove the TAD.
These are just a couple examples of specialized tools an orthodontist can use for bite correction. Thanks to them and similar devices, even the most complex bite problem can be overcome to create a healthier and more attractive smile.
If you would like more information on correcting a poor bite, please contact us or schedule an appointment for a consultation. You can also learn more about this topic by reading the Dear Doctor magazine article “Orthodontic Headgear & Other Anchorage Appliances.”

Pediatricians and dentists alike recommend beginning your child's regular dental visits at an earlier age rather than later. Most say children's first visits should happen around their first birthday.
Some may question whether that's necessary given the state of a child's dental development at that age. At that stage they normally have only a few primary teeth, which will eventually give way to their permanent set soon enough.
But regular dental visits can make a positive difference even at that early age. Here are 3 oral health areas that could benefit from seeing the dentist by Age One.
Protecting primary teeth from decay. It's true that primary teeth don't last long when compared to a normal lifespan. But during their short tenure, they do play a critical role in a child's health and development. Not only do they provide a child dental function for eating, speaking and smiling, they also preserve the space for the permanent teeth that will succeed them. Without them, permanent teeth can erupt out of position to form a poor bite (or malocclusion). That's why early dental care to prevent and treat decay in primary teeth helps them remain for as long as they should.
Detecting developing malocclusions. A malocclusion doesn't form overnight—there can be subtle signs of its development during early childhood. A dentist, especially a pediatric dentist or orthodontist, can often detect those signs before the malocclusion fully develops (one reason why every child should have an orthodontic evaluation around age 6). With early detection, an orthodontist can use interventional techniques that will lessen or even stop a malocclusion from forming. As a result, later orthodontic treatment may not be as extensive—or expensive—as it could have been.
Developing a healthy dentist-patient relationship. Dental anxiety is a real problem for many adults—in some cases it can be so severe they avoid professional dental care altogether. The roots of that dental fear often go back to unpleasant experiences during childhood. Starting dental visits when a child is very young appears to minimize the development of dental anxiety. A young child, especially visiting a "kid-friendly" dental clinic, will more likely view dental care as a routine part of life and will less likely be afraid.
If you would like more information on dental care for children, please contact us or schedule an appointment for a consultation. You can also learn more about this topic by reading the Dear Doctor magazine article “Age One Dental Visit: Why It's Important for Your Baby.”

While the sport of golf may not look too dangerous from the sidelines, players know it can sometimes lead to mishaps. There are accidents involving golf carts and clubs, painful muscle and back injuries, and even the threat of lightning strikes on the greens. Yet it wasn’t any of these things that caused professional golfer Danielle Kang’s broken tooth on the opening day of the LPGA Singapore tournament.
“I was eating and it broke,” explained Kang. “My dentist told me, I've chipped another one before, and he said, you don't break it at that moment. It's been broken and it just chips off.” Fortunately, the winner of the 2017 Women’s PGA championship got immediate dental treatment, and went right back on the course to play a solid round, shooting 68.
Kang’s unlucky “chip shot” is far from a rare occurrence. In fact, chipped, fractured and broken teeth are among the most common dental injuries. The cause can be crunching too hard on a piece of ice or hard candy, a sudden accident or a blow to the face, or a tooth that’s weakened by decay or repetitive stress from a habit like nail biting. Feeling a broken tooth in your mouth can cause surprise and worry—but luckily, dentists have many ways of restoring the tooth’s appearance and function.
Exactly how a broken tooth is treated depends on how much of its structure is missing, and whether the soft tissue deep inside of it has been compromised. When a fracture exposes the tooth’s soft pulp it can easily become infected, which may lead to serious problems. In this situation, a root canal or extraction will likely be needed. This involves carefully removing the infected pulp tissue and disinfecting and sealing the “canals” (hollow spaces inside the tooth) to prevent further infection. The tooth can then be restored, often with a crown (cap) to replace the entire visible part. A timely root canal procedure can often save a tooth that would otherwise need to be extracted (removed).
For less serious chips, dental veneers may be an option. Made of durable and lifelike porcelain, veneers are translucent shells that go over the front surfaces of teeth. They can cover minor to moderate chips and cracks, and even correct size and spacing irregularities and discoloration. Veneers can be custom-made in a dental laboratory from a model of your teeth, and are cemented to teeth for a long-lasting and natural-looking restoration.
Minor chips can often be remedied via dental bonding. Here, layers of tooth-colored resin are applied to the surfaces being restored. The resin is shaped to fill in the missing structure and hardened by a special light. While not as long-lasting as other restoration methods, bonding is a relatively simple and inexpensive technique that can often be completed in just one office visit.
If you have questions about restoring chipped teeth, please contact us or schedule an appointment for a consultation. You can learn more by reading the Dear Doctor magazine articles “Porcelain Veneers” and “Artistic Repair of Chipped Teeth With Composite Resin.”